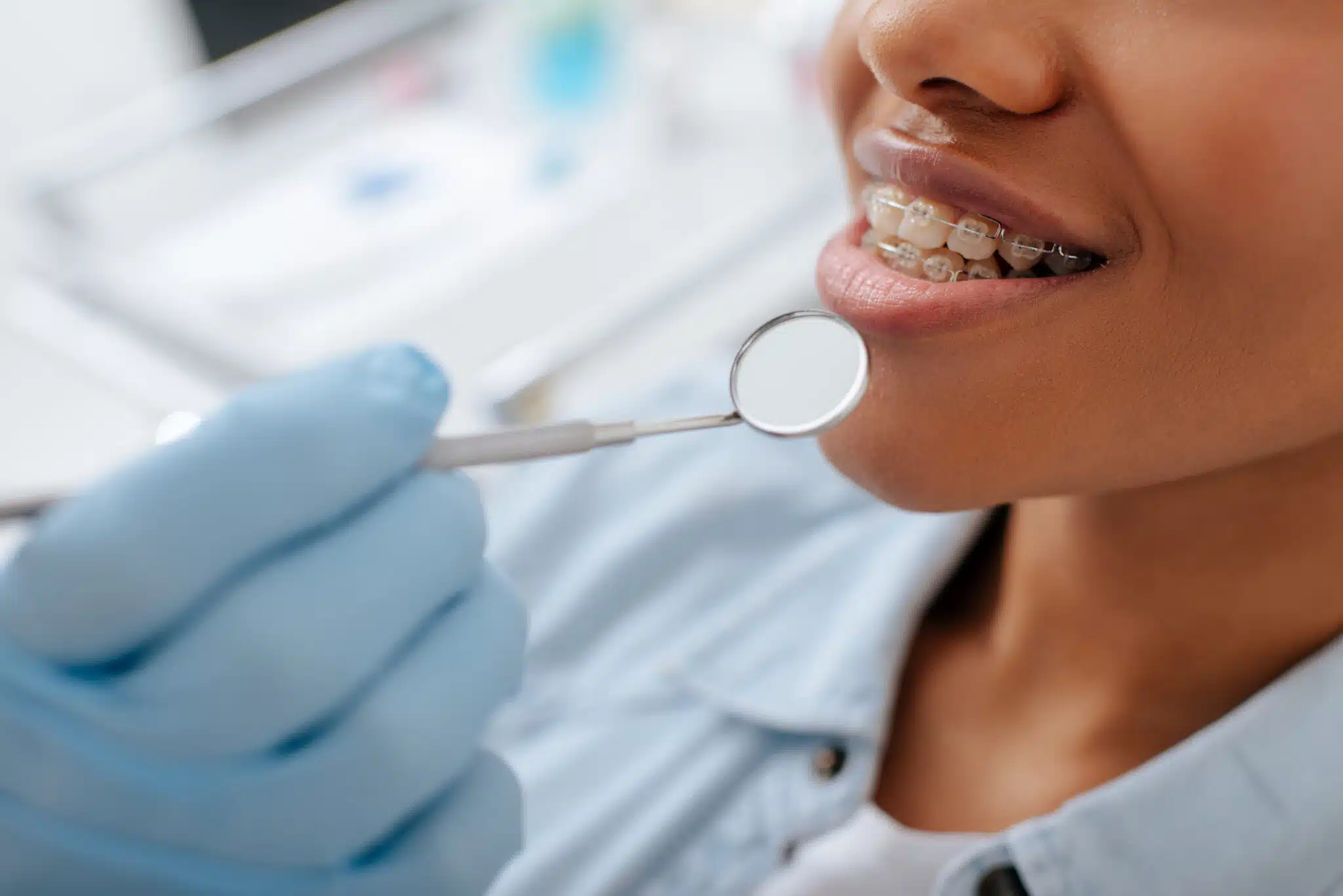
Braces can be a major expense, which is why many people start by asking whether insurance can lower the cost. The answer is sometimes yes, but the details matter. Orthodontic coverage is often limited, and many plans only pay part of the total cost. That means it is important to understand the rules before treatment starts.
For a money-focused audience, the real question is not just whether braces are covered. It is how to use the policy well enough to avoid surprises, compare options, and plan for the out of pocket portion before treatment begins.
How Braces Coverage Usually Works
Orthodontic coverage is often part of a broader dental insurance plan rather than a standalone benefit. A plan may help pay for braces, but the member is still responsible for a share of the cost. Coverage can vary a lot from one policy to another.
This also means braces coverage usually works differently from a routine cleaning or filling. A plan may require a deductible first. It may cover only a percentage of the orthodontic bill after that. Some plans also require preapproval before treatment begins so the insurer can confirm what is covered.
In practical terms, insurance may lower the total cost, but it rarely makes braces inexpensive. The patient still needs a clear estimate of what the insurer will pay and what amount will remain their responsibility.
Why Age Rules and Plan Limits Matter
One of the biggest issues with braces coverage is that not every plan treats adults and children the same way. Some policies focus mainly on children and teens, while others extend orthodontic benefits to adults.
This matters because many people assume braces are covered the same way for everyone on the plan. That is often not true. If orthodontic treatment is being considered for an adult, the first step should be confirming that the policy even includes adult orthodontic benefits. Otherwise, a person may spend time planning around coverage that is not available.
Plan limits matter too. Many orthodontic benefits come with a lifetime maximum. This means the insurer will only pay up to a fixed amount for braces. Once that cap is reached, any additional costs fall to the member. For budgeting purposes, this is one of the most important details in the policy because braces often cost much more than the maximum benefit.
What to Check Before Treatment Starts
Before treatment begins, there are a few details that should be reviewed closely. First, confirm what types of braces are covered. Some plans may cover traditional metal braces but place stricter limits on ceramic braces or clear aligners.
Second, confirm the percentage the plan pays. A policy that covers half the treatment cost may sound strong, but it still leaves half the bill for the patient. Third, check whether there is a waiting period. If treatment needs to start soon, that delay can make the policy far less useful.
Fourth, ask whether the orthodontist must be in network. Even when a plan includes braces coverage, network rules can affect the actual price. Fifth, request a written estimate before approving treatment. That estimate should show the full cost, the expected insurance contribution, and the payment plan for the remaining balance.
These steps can prevent confusion later. They also make it easier to compare treatment options without guessing about cost.
How to Budget for the Part Insurance Will Not Cover
This is where the financial side becomes especially important. Even strong braces coverage usually leaves a meaningful out of pocket cost. A good approach is to treat braces like a planned healthcare expense rather than an emergency bill.
Start with the total treatment estimate. Subtract the amount insurance is expected to pay. Then build a realistic plan for the rest. That may include a payment plan through the orthodontist, dedicated monthly savings, or timing treatment around other large expenses.
Some people search broadly for vision and dental insurance and assume a bundled policy will provide strong support for orthodontic care. In reality, braces coverage is usually determined by the dental portion of the plan, and the orthodontic rules need to be reviewed on their own. Looking closely at those dental details is much more useful than assuming the bundle automatically covers braces in a meaningful way.
How to Compare Plans More Carefully
If you are shopping for coverage before treatment starts, comparing plans side by side can save money later. A lower premium is not always the better value if the braces benefit is weak or unavailable for your age group. A higher premium may still be worthwhile if it offers adult orthodontic coverage, a better payment percentage, and a more usable lifetime maximum.
A smarter comparison looks at the full cost picture. Review age eligibility, treatment types, coverage percentages, waiting periods, network rules, and benefit caps. These details often matter more than marketing language.
It is also helpful to think about timing. If braces are likely within the next year, waiting periods and first-year limits become more important. If treatment is still further away, you may have more time to choose a policy with better long term value.
What Families and Older Adults Should Keep in Mind
Braces are often discussed as a treatment for children and teens, but adults may need orthodontic care too. In some cases, treatment is tied to bite issues, crowded teeth, or preparation for other dental work. That is why it helps to look at coverage with a practical mindset rather than assuming braces are only a cosmetic choice.
Families should focus on how the plan supports dependents and what portion of treatment is realistically covered. Older adults should focus on whether adult orthodontic care is included at all. In both cases, the policy should be judged by what it actually helps pay for, not by what its name suggests.
It is also worth remembering that treatment can last a long time. A plan that looks useful at the start may feel less helpful if the lifetime maximum is reached early or if follow-up costs continue after the main benefit has been used.
Making a Better Braces Coverage Decision
Insurance can help with braces, but only when the policy details line up with the treatment you need. Coverage percentages, age rules, waiting periods, lifetime maximums, and treatment exclusions can all affect whether a plan truly lowers costs in a meaningful way.
The best approach is straightforward. Confirm eligibility, check the type of braces covered, ask for preapproval when needed, and plan for the portion insurance will not pay. When that insurance review is combined with a realistic budget, braces become easier to manage and much less likely to create an unexpected financial strain.